Prostate Artery Embolization (PAE)
Prostate Artery Embolization (PAE) is a minimally invasive medical procedure used to treat a common condition called benign prostatic hyperplasia (BPH), which involves the enlargement of the prostate gland in men as they age. This enlargement can lead to bothersome urinary symptoms like frequent urination, weak urine flow, difficulty starting or stopping urination, and the feeling of not fully emptying the bladder.
During a PAE procedure, a specially trained doctor called an interventional radiologist uses a thin, flexible tube called a catheter to access the blood vessels that supply the prostate gland with blood. This is typically done through a small incision in the groin area. With the help of advanced imaging, the doctor guides the catheter to the right place.
Once the catheter is in the correct position, tiny particles are released into the blood vessels that feed the prostate. These particles are designed to block or reduce blood flow to the prostate tissue, causing it to shrink over time. By making the prostate smaller, the pressure on the urethra (the tube that carries urine from the bladder out of the body) is relieved, which leads to improved urinary symptoms.
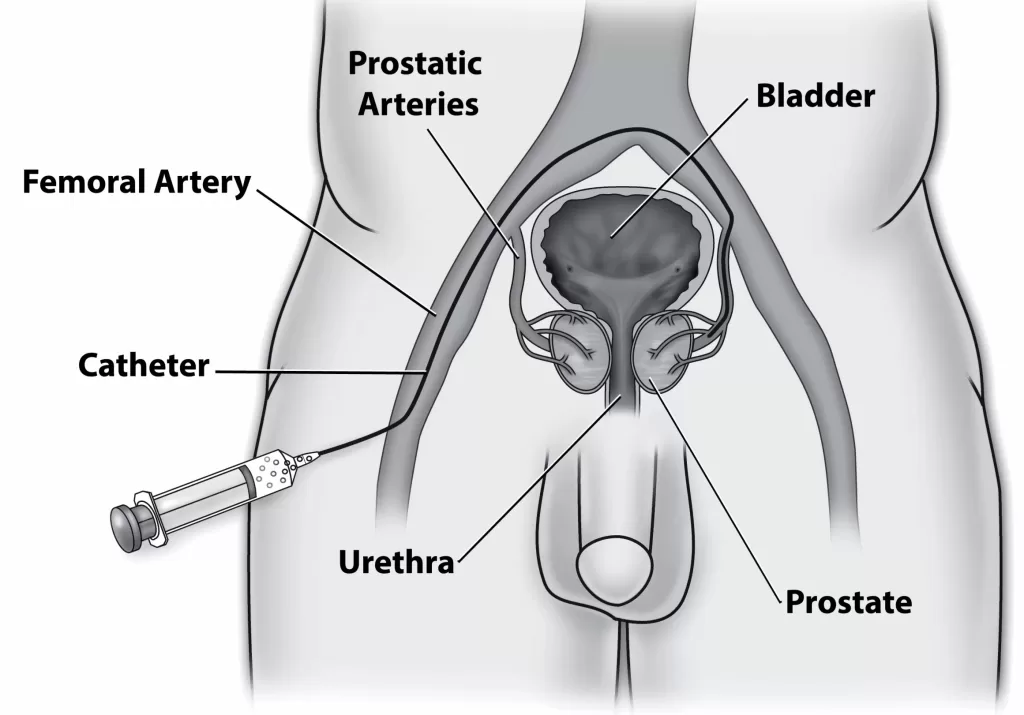
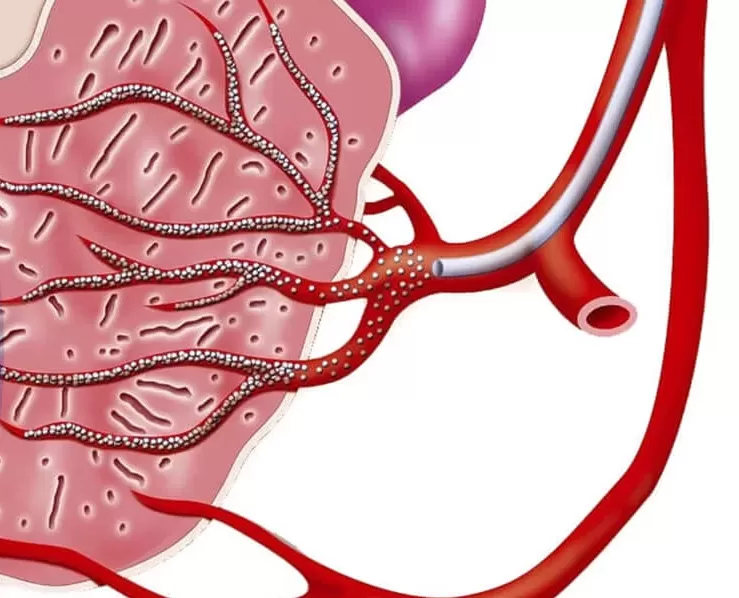
An interventional radiologist is a medical specialist who uses minimally invasive imaging-guided procedures to diagnose and treat various conditions. They are trained in both radiology and interventional procedures, combining their expertise in medical imaging with therapeutic interventions.
Interventional radiologists perform a wide range of procedures using advanced imaging techniques such as fluoroscopy, ultrasound, and computed tomography (CT). These procedures are typically less invasive than traditional surgery and often require only a small incision or needle puncture.
By utilizing image guidance, interventional radiologists can precisely target and treat conditions while minimizing the risks and recovery time associated with open surgery. They work collaboratively with other healthcare professionals to provide comprehensive patient care and offer minimally invasive treatment options for various diseases and conditions.
Benign Prostatic Hyperplasia (BPH) is a common condition in aging men where the prostate gland, located beneath the bladder, grows larger than usual. This non-cancerous enlargement can press against the urethra, which carries urine, causing various urinary problems. Hormonal changes, specifically an increase in dihydrotestosterone, contribute to this growth.
Benign Prostatic Hyperplasia (BPH) can lead to various urinary symptoms due to the enlargement of the prostate gland. These symptoms occur as the enlarged prostate presses against the urethra, which is the tube that carries urine from the bladder out of the body.
Common symptoms of BPH include:
- Frequent Urination: Needing to urinate more often than usual, especially during the night. This can disrupt sleep and daily activities.
- Urgency: Experiencing sudden, strong urges to urinate that can be difficult to control. This can lead to hurried trips to the restroom.
- Weak Urine Stream: The force of the urine stream may be reduced, resulting in a slower or weaker flow.
- Difficulty Initiating Urination: Struggling to start the flow of urine. This might require extra effort and time.
- Incomplete Emptying: Feeling as though the bladder is not fully emptied after urination. This sensation can be bothersome and lead to more frequent trips to the restroom.
- Dribbling: After urination, some urine may continue to leak, causing dampness and discomfort.
- Straining: Experiencing the need to push or strain to initiate or complete urination.
- Urinary Tract Infections: BPH can lead to a higher risk of urinary tract infections (UTIs) due to incomplete bladder emptying.
These symptoms can vary in severity from person to person and can have a significant impact on daily life, affecting everything from sleep quality to social activities.
Treatment options for symptomatic Benign Prostatic Hyperplasia (BPH) aim to alleviate urinary symptoms caused by the enlarged prostate. The choice of treatment depends on the severity of your symptoms, overall health, and personal preferences. Here are common approaches:
Watchful Waiting: For mild symptoms, observation may be recommended.
Medications: Several medications are available to manage BPH symptoms. Alpha-blockers relax muscles around the prostate and bladder neck, improving urine flow. 5-alpha reductase inhibitors reduce the size of the prostate over time. Combination therapy can also be effective. Some patients may not tolerate medications due to side effects of low blood pressure and dizziness.
Trans-Arterial Procedures: Minimally invasive procedures like Prostate Artery Embolization (PAE) aim to shrink the prostate by reducing its blood supply. These are performed by a doctor called an Interventional Radiologist. This can improve urinary symptoms without the need for surgery.
Trans-Urethral Procedures: Several different procedures exist that mechanically remove excess prostate tissue from inside the urethra.
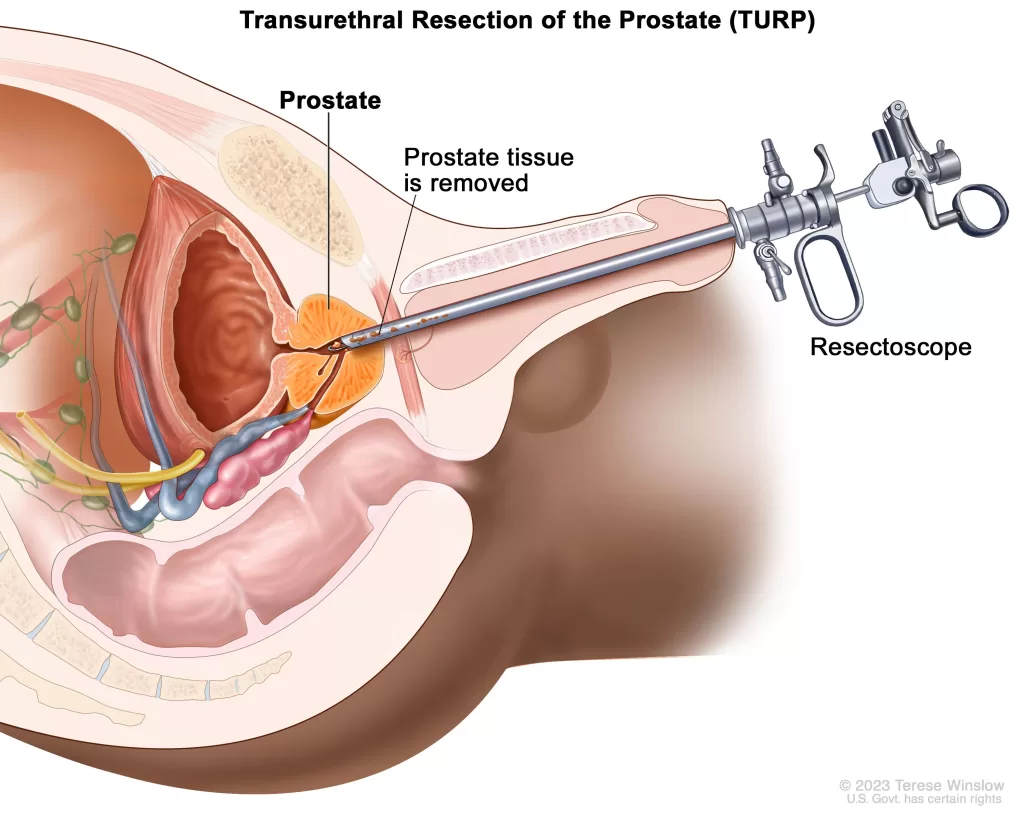
These are performed by a doctor called a Urologist. Transurethral Resection of the Prostate (TURP) involves mechanically scraping excess prostate tissue away. It is the most studied and effective option for treating symptomatic BPH, but also has a higher rate of side effects. Laser treatments like Photoselective Vaporization of the Prostate (PVP) and Holmium Laser Enucleation of the Prostate (HoLEP) use laser energy to remove excess tissue or vaporize it from inside the urethra. Newer procedures such as Rezum remove tissue by using water vapor or steam. Alternatively, a Urolift procedure uses a permanent implant anchor placed from inside the ureter to hold the excess prostate tissue out of the way.
Open Surgery: In severe cases, when other treatments aren’t effective or if complications arise, open surgery like a simple prostatectomy might be considered to relieve urinary obstruction.
It’s important to consult a urologist and/or interventional radiologist to discuss the most suitable option for your situation. The decision should consider your symptoms, medical history, preferences, and potential risks and benefits. Early intervention can help improve your quality of life by relieving bothersome urinary symptoms associated with BPH.
Treatment for Benign Prostatic Hyperplasia (BPH) can involve different approaches, each tailored to the patient’s condition and preferences. Prostate Artery Embolization (PAE) and transurethral procedures are two distinct options, differing in technique, invasiveness, and recovery.
Prostate Artery Embolization (PAE): PAE is a minimally invasive procedure. It involves a catheter inserted through a small incision in the groin, guided to the arteries supplying the prostate. Microscopic particles are introduced to block blood flow to the prostate, causing it to shrink. This reduction relieves pressure on the urethra, easing urinary symptoms. PAE typically leads to shorter hospital stays, less discomfort, and quicker recovery compared to traditional surgeries.
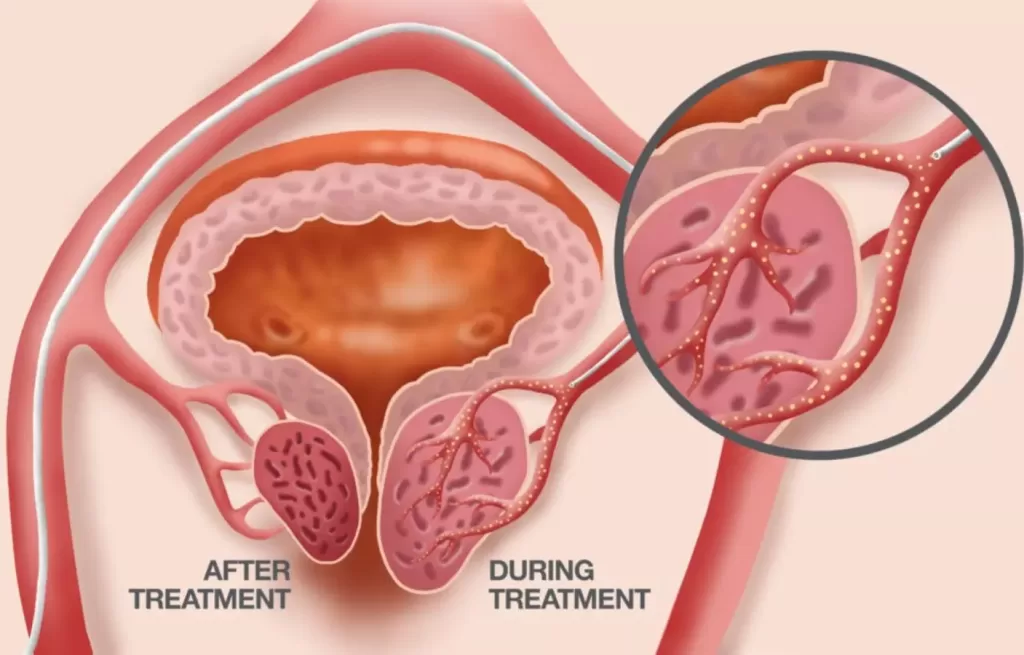
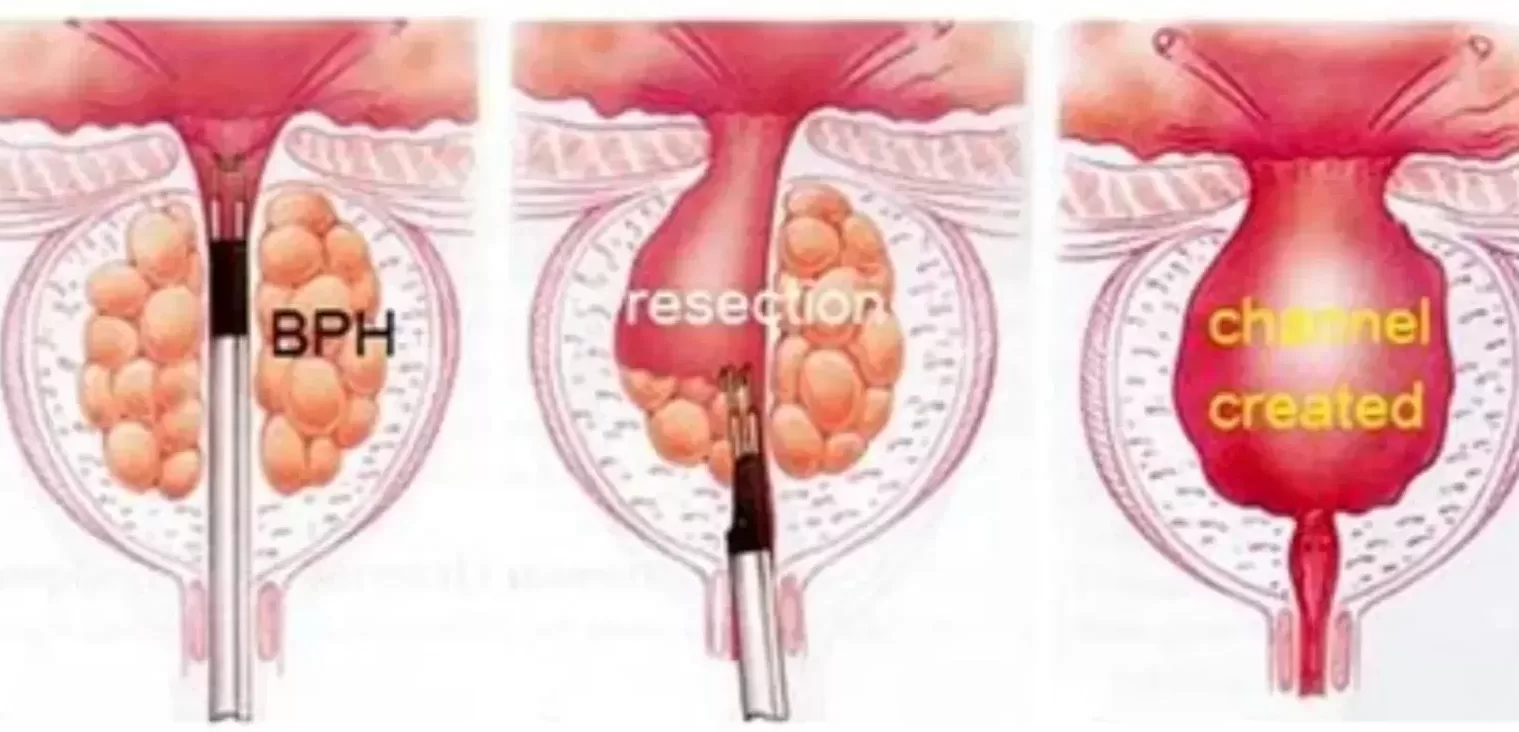
Transurethral Procedures: Transurethral procedures are more invasive and involve interventions through the urethra. Transurethral Resection of the Prostate (TURP) involves removing excess prostate tissue to improve urine flow. Transurethral Incision of the Prostate (TUIP) involves making incisions to widen the urethra. These procedures often require general or spinal anesthesia, and recovery times can be longer than with PAE.
Key Differences:
- Invasiveness: PAE is minimally invasive, involving only small incisions for catheter placement. Transurethral procedures are more invasive, involving entry through the urethra and removal of tissue.
- Anesthesia: PAE is usually performed under local anesthesia. Transurethral procedures typically require general or spinal anesthesia, which carries its own set of risks.
- Hospital Stay: PAE generally leads to shorter hospitalization compared to transurethral procedures.
- Recovery: Recovery from PAE is often quicker, with less discomfort. Transurethral procedures might involve more postoperative discomfort and a longer recovery period.
- Patient Suitability: PAE might be suitable for patients who are not candidates for traditional surgeries due to factors like age or health conditions.
- Long-Term Data: PAE is a newer procedure, and its long-term outcomes are still being studied. Transurethral procedures have a longer track record.
The choice between PAE and transurethral procedures depends on various factors, including the severity of BPH symptoms, overall health, and patient preferences. While PAE offers the advantage of being minimally invasive and leading to quicker recovery, transurethral procedures have established efficacy in managing BPH over a longer period. Consulting a urologist and/or interventional radiologist can help determine the most appropriate treatment approach for an individual’s unique situation.
On average, UAE typically takes around 2 hours to complete. However, it’s important to note that this is an estimate, and the actual time can vary.
In most cases, PAE is performed under conscious sedation & local anesthesia.
Conscious sedation involves the administration of medications to help you relax and feel drowsy during the procedure. You may be in a semi-conscious state and still able to respond to instructions and communicate with the medical team.
Local anesthesia is used to numb the area where the catheter is inserted, typically in the groin region. This ensures that you don’t feel pain or discomfort during the procedure.
General anesthesia, which puts you completely asleep, is generally not required for PAE unless there are specific medical considerations or additional procedures being performed in conjunction with the embolization.
In general, PAE does not require placement of a catheter through the urethra into the bladder. In a small number of cases, however, placing a temporary catheter may facilitate a successful procedure. In these situations, the catheter is removed immediately following the procedure before going home.
Recovery following Prostate Artery Embolization (PAE) is generally well-tolerated and often more comfortable compared to traditional surgical approaches. Here’s what you can expect during the recovery period:
- Immediately Post-Procedure: After the PAE procedure, you will likely spend a few hours under observation in a recovery area. Medical staff will monitor your vital signs and make sure you are comfortable.
- Discharge: In many cases, patients are discharged on the same day as the procedure. However, some observation time might be required depending on individual circumstances.
- Pain and Discomfort: You might experience mild discomfort or soreness at the groin incision site where the catheter was inserted. Over-the-counter pain relievers are often sufficient to manage this discomfort.
- Activity: You’ll be encouraged to resume light activity within a day or two after the procedure. Walking and gradually increasing your activity level can help prevent blood clots and aid in recovery.
- Urinary Symptoms: It’s common to experience some initial urinary symptoms, such as increased frequency or urgency, as your body adjusts to the changes in the prostate. These symptoms typically improve over the coming weeks.
- Follow-Up: You’ll have a follow-up appointment with your healthcare provider to assess your progress and discuss any concerns you might have. This appointment is an opportunity to review your recovery and address any questions you might have about your ongoing care.
- Return to Normal Activities: Many patients are able to return to their normal activities, including work, within a few days to a week after the procedure. However, it’s important to avoid heavy lifting and strenuous activities for a couple of weeks to allow your body to fully heal.
- Long-Term Improvement: Over the course of several weeks to months, you should start to notice a gradual improvement in your urinary symptoms. As the prostate continues to shrink, the pressure on the urethra decreases, leading to better urinary flow and reduced symptoms.
- Monitoring: We will continue to monitor your progress over time to ensure that the desired outcomes are achieved. This might involve additional follow-up appointments and possibly imaging studies to assess the prostate’s response to the procedure.
It’s important to follow your post-procedure instructions closely and attend all scheduled follow-up appointments. While recovery after PAE is generally smoother than traditional surgical methods, every patient’s experience is unique.
Yes, you will need someone to drive you home following your procedure.
It is also a good idea to have someone stay with you for the first couple of nights to help manage pain and medications just in case your symptoms are severe.
Prostate Artery Embolization (PAE) is generally considered safe, but like any medical procedure, it does carry some risks. It’s essential to understand these potential risks and discuss them with your healthcare provider before undergoing the procedure. Here are some of the possible risks associated with PAE:
Infection: Although the risk is generally low, it’s important to monitor for signs of infection, such as fever, pain, or increased redness at the incision site.
Bleeding: There may be minor bleeding or bruising at the catheter insertion site in the groin. This usually resolves on its own but should be monitored.
Prostate Inflammation: As the prostate responds to the embolization, some inflammation may occur. This can lead to temporary worsening of urinary symptoms before improvement occurs.
Urinary Retention or Incontinence: While uncommon, there’s a slight risk of temporary urinary retention (difficulty emptying the bladder) or incontinence (involuntary urine leakage). Rarely, a catheter may need to be inserted to help drainage.
Non-Target Embolization: In rare cases, the particles used in embolization could inadvertently block blood vessels in unintended areas, which might lead to damage or complications.
It’s important to note that while these risks exist, they are relatively uncommon. Your healthcare provider will conduct a thorough assessment of your medical history and health status to determine if you’re a suitable candidate for PAE. They will also discuss these risks with you and provide guidance on how to mitigate them.
If you have concerns about the risks associated with PAE or want to learn more about the procedure’s potential benefits, make sure to have an open and thorough discussion with your healthcare provider. They can help you make an informed decision about whether PAE is the right choice for your specific situation.
Yes, Prostate Artery Embolization (PAE) is generally associated with preserving sexual function better than certain surgical methods for treating Benign Prostatic Hyperplasia (BPH). While individual experiences may vary, PAE aims to minimize the risk of sexual side effects. Temporary changes, such as altered ejaculation patterns or reduced libido, might occur initially, but these typically resolve over time. Compared to procedures involving tissue removal, PAE’s impact on sexual function is generally less pronounced and of shorter duration. It’s important to discuss any concerns about sexual function with your healthcare provider before the procedure to gain personalized insights based on your situation.
After undergoing Prostate Artery Embolization (PAE), the timeline for experiencing improvements in your symptoms can vary. While some men may notice changes relatively quickly, it’s important to understand that individual responses to the procedure can differ, and several factors may influence the speed at which you see results.
In the days following PAE, you might experience some initial changes in your urinary symptoms. These could include a gradual improvement in urinary flow, reduced urgency, and less frequent nighttime urination. However, it’s common for the full benefits of the procedure to become more noticeable over a period of several weeks to months.
As the prostate gland responds to the embolization and begins to shrink, the pressure on the urethra decreases. This often leads to a progressive reduction in urinary symptoms over time. Many men experience improvements in weak urine flow, frequent urination, urgency, and the feeling of incomplete bladder emptying.
It’s essential to be patient and allow your body the time it needs to respond to the treatment. Keep in mind that the rate of improvement can vary based on factors such as the size of the prostate, the severity of your symptoms, and your body’s unique healing process.
Yes, Prostate Artery Embolization (PAE) has been demonstrated to be an effective treatment for relieving the urinary symptoms associated with Benign Prostatic Hyperplasia (BPH). Numerous clinical studies and real-world experience have shown positive outcomes and symptom improvement in patients who undergo PAE.
Clinical research evaluating PAE’s efficacy has consistently shown that it leads to a reduction in urinary symptoms caused by BPH. Studies have reported improvements in symptoms such as frequent urination, weak urine flow, urgency, and incomplete bladder emptying. Many patients experience a significant enhancement in their overall quality of life after undergoing PAE.
Furthermore, PAE has been found to have a favorable safety profile. Complications are generally rare, and the procedure’s minimally invasive nature contributes to quicker recovery times compared to traditional surgical approaches. Patients often experience less discomfort, shorter hospital stays, and faster returns to their normal activities.
It’s important to note that while PAE has demonstrated its effectiveness in relieving BPH symptoms, individual responses can vary. Factors such as the severity of symptoms, the size of the prostate, and the patient’s overall health can influence the specific outcomes.
Yes, Prostate Artery Embolization (PAE) is particularly well suited for certain groups of patients who are seeking a minimally invasive alternative for the treatment of Benign Prostatic Hyperplasia (BPH). PAE offers benefits that make it especially attractive for these specific patients:
- High Surgical Risk: Patients who are at a higher risk for complications from traditional surgery due to age, existing medical conditions, or other factors might find PAE to be a safer option. PAE’s minimally invasive nature reduces the risks associated with major surgery.
- Desire to Avoid Surgery: Some patients prefer to avoid traditional surgical methods and the associated risks, discomfort, and longer recovery times. PAE offers an effective alternative that often results in quicker recovery and less disruption to daily life.
- Multiple Health Issues: Patients who have various health conditions that might complicate surgery might be better suited for PAE. Since PAE doesn’t require major anesthesia or invasive surgery, it can be a more feasible option for individuals with multiple health concerns.
- Large Prostate Size: PAE can be particularly effective for patients with larger prostates that might pose challenges for traditional surgical procedures. The procedure’s goal of reducing prostate size can lead to significant symptom improvement in these cases.
- Medications Not Effective: Patients who have tried medications to manage BPH symptoms but found them to be ineffective or associated with unwanted side effects might consider PAE as an alternative solution.
- Patient Preference: Some individuals simply prefer minimally invasive approaches and a faster return to their regular activities. PAE’s shorter hospital stay and quicker recovery align with their preferences.
- Desire to Preserve Sexual Function: Many men who undergo PAE report minimal disruption to their sexual function and even mild improvement. In fact, PAE is associated with a lower risk of sexual side effects compared to procedures that involve the removal of prostate tissue, such as Transurethral Resection of the Prostate (TURP).
- Catheter Dependent Patients: For some patients with severe BPH, long-term catheters are required for urinary drainage. In these patients, PAE can sometimes facilitate prostate shrinking and eventual catheter removal.
It’s important to emphasize that while PAE is well suited for these groups, individual circumstances vary. Consulting with a qualified healthcare provider is essential to determine if PAE is the appropriate treatment option based on your medical history, symptoms, and overall health. Your healthcare provider will provide personalized guidance to help you make an informed decision about the best course of action for managing your BPH symptoms.
Unfortunately, no. Prostate Artery Embolization (PAE) is not a suitable treatment for prostate cancer. PAE is specifically designed to treat benign conditions such as Benign Prostatic Hyperplasia (BPH), which involves the non-cancerous enlargement of the prostate gland.
